Where the SRT Fits in Real-World Biomechanics & Gait Assessment
The supination resistance test (SRT), often called a “resupination” test, is a simple, weight-bearing manual assessment that asks one main question: how much force does it take to get this foot to start supinating under load?
In our biomechanics and gait teaching, that question matters because it shifts the conversation from “foot shape” to force and function—what moves, how it moves during stance and gait, and where the load is likely being absorbed.
Many clinicians were taught to focus heavily on static foot posture (“flat” vs “high arch”) and then jump straight to an orthotic prescription. If that was your experience, the SRT is a helpful upgrade. It gives you a quick sense of how much resistance you’re working against when you try to change foot motion under body weight.
SRT in One Minute: What It Is (and What It Isn’t)
- It is: a quick estimate of how much upward force is needed to initiate supination or arch rise while the patient is standing.
- It isn’t: a “pronation severity score,” a diagnosis, or a guarantee that orthoses will (or won’t) work.
- It helps you: choose a realistic intervention dose and set expectations.
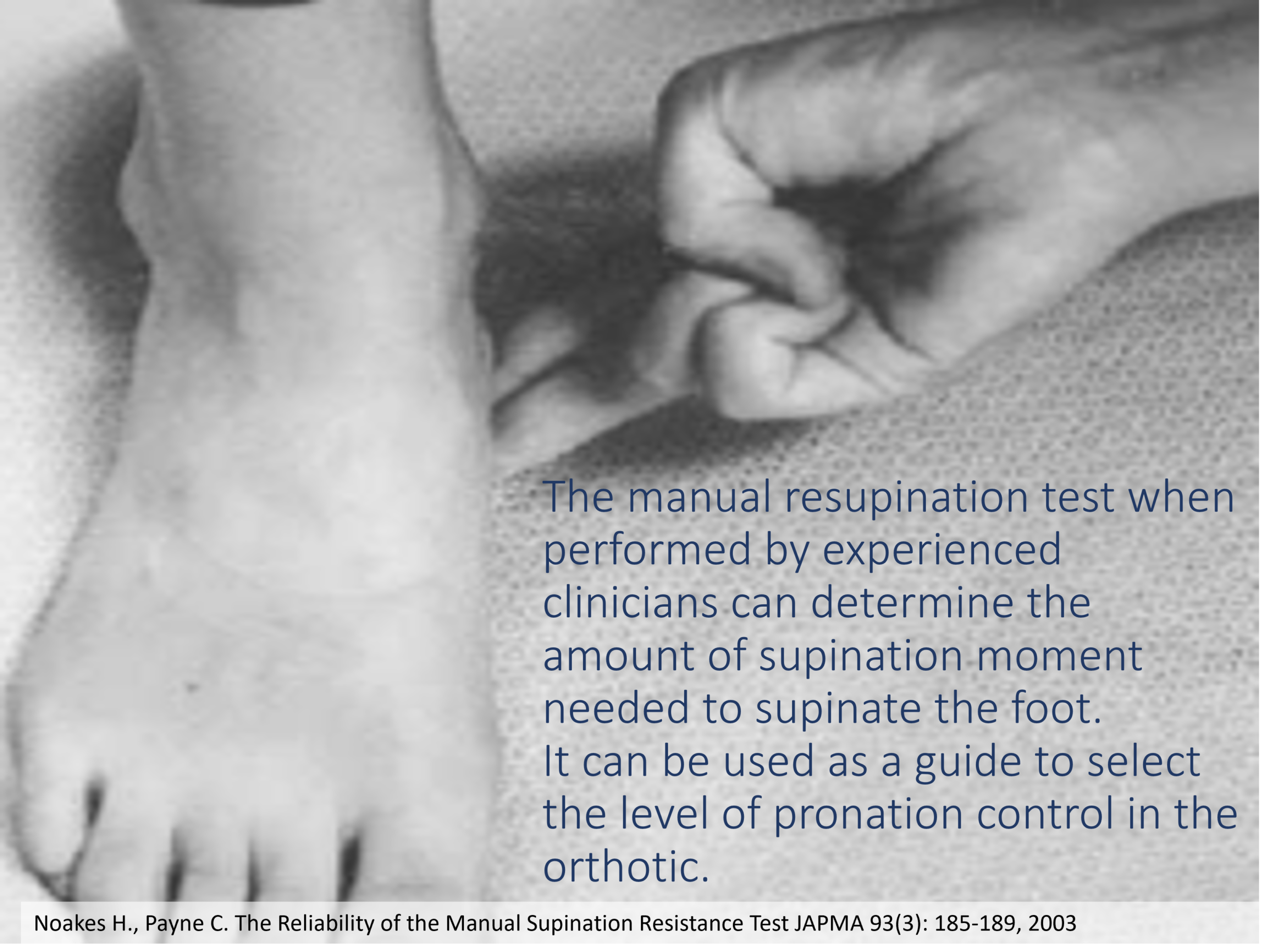
History in Brief: Kirby, Payne, and the Evolution of SRT
The SRT is widely attributed to Kevin A. Kirby, DPM, and is commonly traced to early podiatry biomechanics writing (Kirby & Green, 1992). Other clinicians and educators, including Craig Payne, have contributed substantially to the literature and teaching around the SRT.
Payne’s research demonstrated that body weight and joint geometry are key factors influencing SRT values. He also published studies showing that the manual SRT is reliable when performed by experienced clinicians.
Later authors, including Ian B. Griffiths and Gabriel Moisan, helped standardise technique, examine reliability, and explore relationships between SRT values, gait biomechanics, and orthotic response.
How to Do the SRT So It’s Repeatable and Teachable
Step-by-step
- Position: relaxed standing posture with natural base and angle of gait.
- Hand placement: index and middle fingers under the medial arch, just plantar to the navicular/talonavicular region.
- Direction of force: upward lift (plantar to dorsal), broadly parallel to the tibia.
- Estimate resistance: judge how much force is required to initiate arch rise.
Practical Tips
- Watch for subtle weight shift.
- Ask patient to relax toes to avoid windlass “cheat.”
- Keep stance width and foot angle consistent.
- Repeat 2–3 times and compare sides.
Common Mistakes New Grads Make (and Quick Fixes)
- Weight shift: cue equal weight; watch pelvis/shoulders.
- Toe gripping: ask for toe relaxation; slight knee bend can help.
- Inconsistent stance: mark foot position if needed.
- Finger placement too distal: reposition under posterior-medial arch.
- Diagonal force: lift vertically.
- Going too hard: apply smooth force until first “give.”
- Only doing it once: repeat 2–3 times.
- Not comparing sides: side-to-side difference is often most useful.
Simple Documentation Framework
Record:
- SRT grade (low, average, high)
- Side-to-side difference
- Your immediate plan
Using the SRT for Orthoses, Footwear and Load Management Decisions
The SRT is most useful as a “dose check” for intervention. High resistance may require stiffer materials or more strategic design; low resistance may call for conservative posting and gradual progression.
- Lower SRT: modest external influence needed; start conservative.
- Higher SRT: stiffer shell or more strategic design may be required.
What Recent Journal Articles Add to the Conversation
Payne: SRT influenced by subtalar joint axis position and body weight; manual SRT reliable with experience.
Moisan et al. (2026): normative values; body mass explains meaningful variation; static posture explains little.
Reliability: multiple studies show SRT is reliable and clinically useful when performed consistently.
Limitations, Pitfalls, and How to Avoid Them
- Partly subjective unless instrumented.
- Easy to “cheat” with subtle compensations.
- Reflects multiple influences (mass, lever arms, stiffness, muscle activity).
- Not a pronation score.
- Should not replace clinical reasoning.
Wrap-Up and Where to Learn This Hands-On
The SRT has lasted because it is fast, intuitive, and fits a force-based way of thinking about foot function. Research from Kirby, Payne, Griffiths, Moisan and others continues to refine how we interpret and apply it.
If you’d like to learn how we integrate the SRT into a full assessment sequence and then connect it to gait observation, orthotic prescription or modification, and practical case reasoning, this is exactly what we teach in Pain Free Feet biomechanics and gait workshops.
